Electronic patient files prevent dangerous drug interactions; telemedicine provides patients access to medical expertise no matter where they are; health apps strengthen the chronically ill. In the digital transformation of the healthcare sector, however, EU Member States are advancing at different speeds. In our #SmartHealthSystems study, which is now published in English, we compared the progress of Digital Health in 14 EU Member States and three OECD countries. Using our specifically developed Digital Health Index, we found three key factors common to the leading countries. In addition, the study provides insights into the ‘lessons learned’ of various countries regarding the implementation of Digital Health into regular healthcare delivery.
On behalf of the Bertelsmann Stiftung, the Bonn based research institute empirica Communication and Technology Research conducted an extensive cross-national study on digitisation strategies and the progress made in 17 different national healthcare systems. Research aimed to identify the countries that have been successful in digitizing their healthcare systems. Particular attention was therefore paid to the strategies pursued by the countries examined and to the lessons that can be drawn from the experience of successful countries.
The study aims to provide more than a simple description of the extent to which digitisation has been adopted within a particular healthcare system. Instead, it focuses on framework conditions, paths taken and success factors, which are specific to each country and can vary widely. Countries of different sizes and with different types of healthcare systems were selected for analysis; they include 14 EU Member States and three OECD countries (i.e., Australia, Canada and Israel).
The Digital Health Index
In the first part of the study, each of the 17 countries was benchmarked and then compared to each other with a new Digital Health Index that was developed specifically for the study. The second part of the study examines five of the 17 countries in greater detail, in order to gain insights about best practices and obstacles to implementing Digital Health.
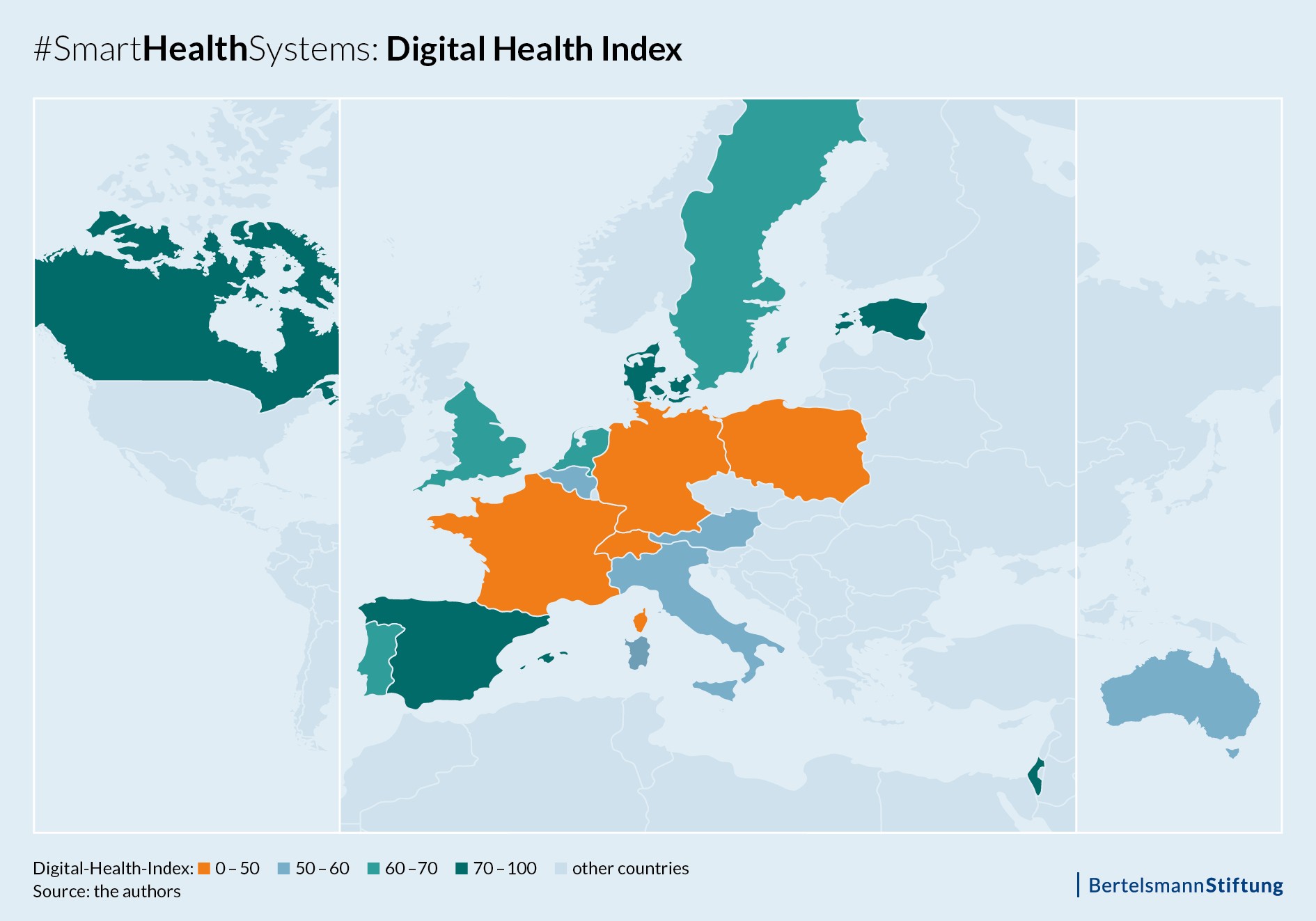
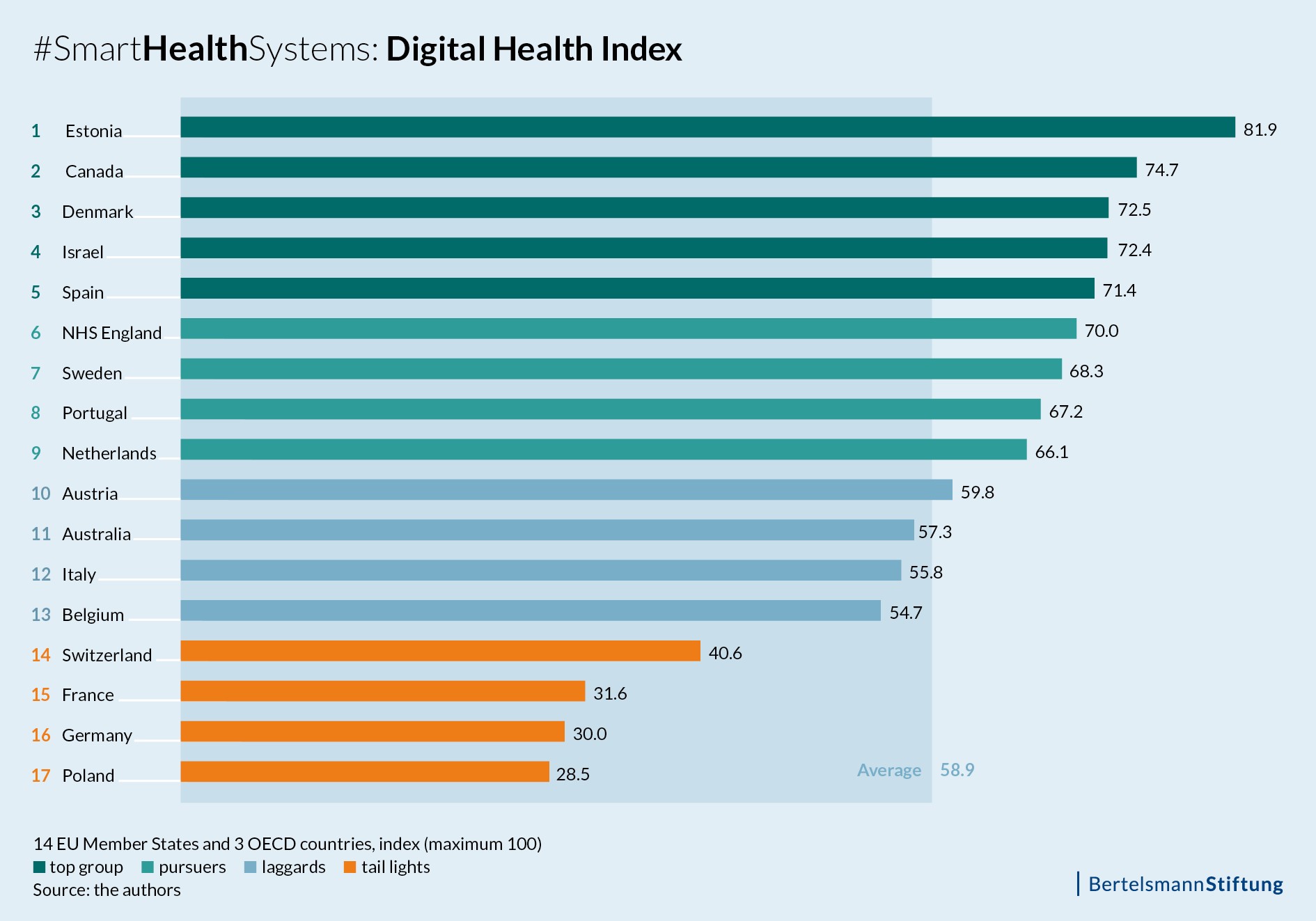
Digital Health Index results are plain and clear: EU Member States and OECD countries digitize their healthcare systems at very different speeds. Estonia, Denmark and Canada rank at the top of the index, whereas France, Germany and Poland trail behind. The top countries of the Index are leading in all three areas examined: policy activity and strategy, technical implementation and readiness as well as the actual use of data.
In the best performing countries Estonia, Canada, Denmark, Israel and Spain, digital technologies are already commonplace in practices and clinics. Prescriptions are for instance transmitted digitally and important patient health data is stored in electronic records, which can be accessed directly by doctors and clinics. In Estonia and Denmark, all citizens can view the results of their examinations, medication plans or vaccination data online. They can manage access for doctors and other healthcare professionals themselves. In Israel and Canada, remote diagnosis and remote video consultations are a part of the regular healthcare delivery.
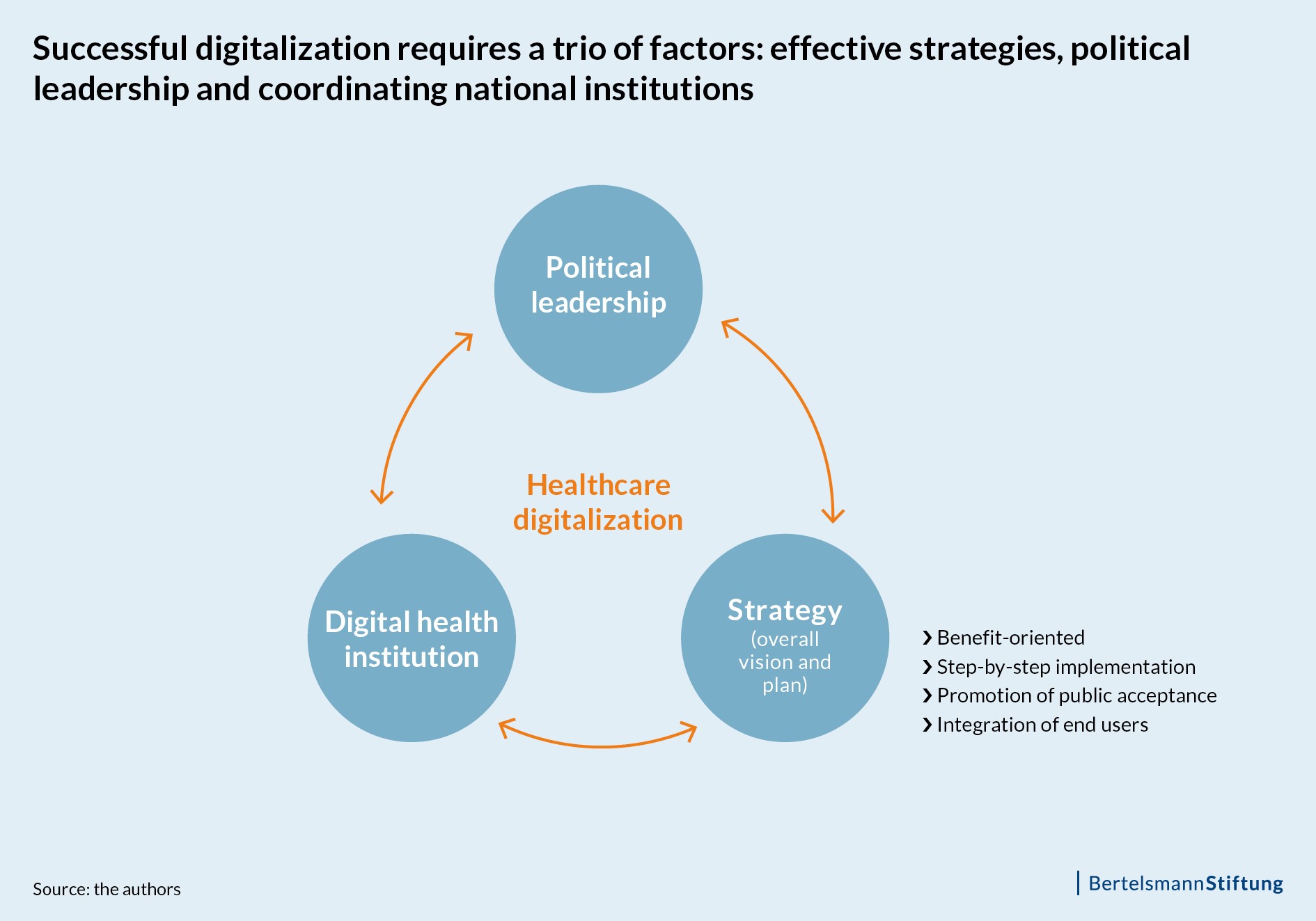
A trio of key success factors in the digitization of healthcare
For a successful digital transformation of the healthcare system, an effective strategy, political leadership and a dedicated institution at national level are required. Successful countries take pragmatic strategic steps and gradually introduce individual processes such as digital prescriptions. Politics should provide a clear framework, ensure acceptance by different stakeholders and drive progress.
Lessons learned
Good health policy involves providing a clear framework that fosters acceptance and drives developments. Digital strategies should be policy oriented according to the needs and imperatives of the individual health system – such as improving quality of care and services, increasing patient safety, or facilitating access to care in rural areas. Advancing digital transformation should focus first on individual, well-prioritized services.
Co-design is an effective means to promoting user acceptance. Resistance to the various change processes triggered by digitisation is a common phenomenon in various countries. As a result, many countries have recognized that promoting acceptance is of strategic importance and that this requires spending adequate resources on communication and dialogue with stakeholders and citizens.
Digital processes and solutions should be tailored to the needs of users. Strategies and digital solutions should be co-designed by end-users and key stakeholders alike whose feedback should be part of development processes.
A well-framed digital health strategy is a signpost and motor for the healthcare sector. To assist EU Member States in pursuing digital reform, already existing national strategies could be promoted EU-wide as potential cross-border role models for driving the respective national uptake of digital solutions.
All study contents and an interactive map can be found at: www.smarthealthsystems.de/en
Click here to subscribe to our newsletter: