As part of our #SmartHealthSystems study which examines the digital transformation of healthcare systems in 17 countries, we have visited five of these countries to take a closer look at what they have achieved. In each country, we have explored the political, cultural, technological and economic factors driving success as well the obstacles to advancing digitization strategies in healthcare. The findings of our cross-national study will be published in November 2018. Until then, we will be highlighting thought-provoking insights and best practices from other countries here in our blog. Denmark and its national health portal sundhed.dk is the first country to be featured in our series.
Denmark has demonstrated an eagerness to invest in new ideas. Take, for example, the country’s cycling infrastructure – broad bicycle-only pathways have long been an integrated feature of many commuter cities in the country. Or the issue of statutory broadcasting fees – which the government has recently announced it plans to do away with and fund public broadcasters via tax income instead.
Denmark has also been quick to promote innovations in the health sector. In the mid-1990s, the national government, together with regions, municipalities and the private sector, began working on “MedCom – The Danish Healthcare Network,” a project designed to develop national standards in order to facilitate data flows between healthcare providers.
This proved to be a crucial investment, as today more than 1.7 million Danes – more than one-fourth of the country’s entire population – visit the site sundhed.dk every month. However, the website, which means “Health” in Danish, is much more than a URL providing health information. Sundhed.dk is a national portal that aims to be the first point of contact for all Danish citizens seeking information about their health.
A national e-health strategy and uniform standards underpin success
Every Dane receives a personal identification number at birth that he or she can use to log in under “My health status” at sundhed.dk. Once logged in, the user has access to an overview of his or her entire health history, including diagnoses, courses of treatment, operations, discharge documents, medication plans, x-ray results and scans, as well as referrals to specialists, immunization records and lab results. The portal serves as a centralized point of access for patients who wish to access all items of information in their electronic health records.
And that’s not all – through sundhed.dk, patients can register as an organ donor, schedule appointments with physicians, request a prescription refill, exchange thoughts and experiences with other patients or inform themselves more generally on health issues and illnesses, as well as their diagnoses and treatments. Most recently, users have begun accessing this information directly through a growing number of apps on their smartphones.
With their patient’s consent, general practitioners or pharmacists can access patient information that has been saved on the portal. They can discuss issues with other healthcare providers and obtain the most recent evidence-based information on specific topics. They can also use the portal to calculate or bill for provided health services.
The number of visitors to the national portal has grown steadily since its launch in 2003. Surveys show 24% of all Danes reporting that treatment has improved as a result of the portal. Some 41% claim that the portal has enhanced their understanding of their condition. And national evaluations show a similarly positive impact: Clinic expenses have been contained and, according to figures provided by sundhed, the national death rate has even fallen.
For many other countries, the Danish national health portal represents a best-practice model for establishing a modern information and communication infrastructure for courses of treatment. The international consultancy and market research firm Gartner highlighted sundhed.dk in 2007 as the best example worldwide of public healthcare information exchange.
Germany, too, is planning to establish a national health portal, though this is still in the early stages (see our “10 Theses” blog post). The German government has been interested in identifying the secret to the Danes’ success in the area of e-health for some time. In 2013, the German Ministry of Health commissioned an in-depth study of the Danish model. The study highlighted two key factors to sundhed.dk’s success: In addition to having pursued a national e-health strategy since the 1990s that found support among all stakeholders in the digital transformation of the healthcare system, the country developed uniform standards for the exchange of data through MedCom and the flow of communication among different actors in the healthcare system.

The gradual development of a complex network
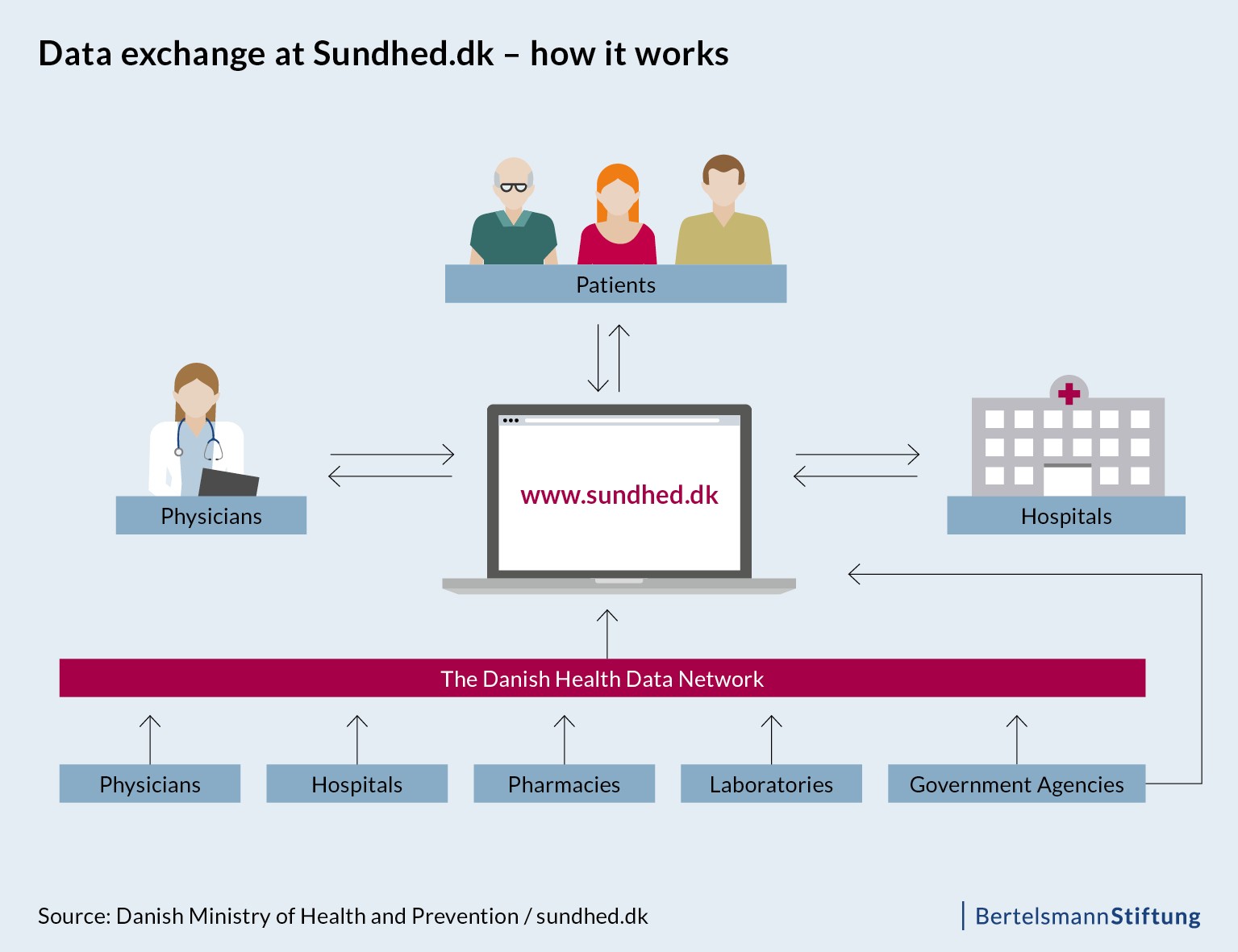
The portal draws on data from a variety of sources that have been linked to the portal. Over the years, Denmark has built up an information and communication infrastructure that allows various actors to collaborate on a single course of treatment. Similar to the plans for Germany’s telematics infrastructure, the data within a patient’s records in the Danish model are stored locally, in different locations. Sundhed.dk thus functions as the platform through which patients, physicians, hospitals and pharmacists can access more than 100 different sources of data.
What may sound simple is, in fact, a complex web of different actors and service providers as well as databases, health registries and IT systems. Work on the system began nearly twenty years ago. MedCom operates the Danish Healthcare Data Network underlying sundhed.dk. As a non-profit organization, MedCom has been commissioned by the Danish Ministry of Health to develop standards for electronic health records that producers of medical practice management software can integrate into their System.
Early standardization, patience and the Danish public’s trust
MedCom was established in 1994 with the launch of a national e-health strategy for Denmark. Even then, at a time when accessing the internet involved dialing up through a modem, Danish hospitals started using electronic health records. At that point, MedCom’s task was to focus on defining interoperability standards for the most common text-based forms of communication such as referrals, clinical or lab reports between public hospitals, medical practices and pharmacies.
However, the standards were rarely used by anyone – initially. During their first year of introduction, only a few thousand messages were exchanged using the new standards. But instead of declaring the project a failure, the Ministry of Health decided to extend MedCom’s contract and to invest in developing the standards even further.
Although it has taken nearly ten years, Denmark can now boast of featuring one the world’s most coherent digital infrastructures for the exchange of electronic health information. Here, too, the statistics underscore a success story: Each year, more than 60 million documents are exchanged across sectors via the Health Data Network. This includes, for example, lab results, 96% of which are sent electronically. The share of prescriptions sent by pharmacies electronically has reached 85 %. And nearly all hospital referrals to physicians are also sent electronically (99%). Overall, sundhed.dk has become the most-used digital tool among physicians.
The gradual expansion of medical data flows across the entire country was made possible in large part by the fact that Denmark’s five regions helped finance up to 80% of the platform’s costs. The remaining 20% came from various ministries and municipalities. The government was thus able to make sure that health directorates in each of the country’s five regions had a shared stake in securing the platform’s success. The five regions also determined which electronic health record systems to implement in their respective area. And although only two out of five regions use the same system, the Danish E-Health Board (which includes representatives from the regions, government and physicians associations) ensures the use of mandatory standards that allow for the exchange of data across regions and through sundhed.dk.
The Danish population has also played an important role in fostering a smooth flow of data across government agencies and other institutions: The Danes generally express greater trust and faith in the state’s competence – including with regard to how data is handled – than do Germans. Surveys show that 80% of Danes are willing to offer more personal data than they have provided – for quite a while now. Since 1977, registering diagnoses, treatments, hospital stays or referrals have been routine in the Danish healthcare system. For Danish patients, electronic health records are nothing new.
Even a good system can be improved upon
As is often the case, even models of success have their downsides. For sundhed.dk, this means that the national portal has become a massive tanker of sorts that is difficult to steer. Aspects of its technical structure and some of its standards date back to the 1990s. And the number of individual standards is steadily growing. For the five regions, 98 municipalities and all physicians involved, adopting the entirety of the standards would require enormous resources. The size of individual patient records is also increasing and contributing to ever-growing mountains of data. The record for an elderly patient with a chronic illness that includes all of their examination results and physicians’ notes can easily reach 500 pages.
But are there patients that will actually read all of that documentation? Physicians, too, are increasingly faced with the challenge of sifting through pages and pages of data in order to obtain an overall view of a complex medical history. In many cases, physicians prefer to prescribe an examination they themselves conduct rather than spend hours reading through files to find the information they need. Many physicians have also expressed frustration with the Danish government’s strict documentation requirements, which often overload medical personnel and are in many cases anything but reasonable and practical.
Of course, the principle of a transparent healthcare system is also subject to criticism. General practitioners in particular have expressed their concerns in this regard, pointing for example to professional secrecy obligations. Should a physician include every intimate detail entrusted to her by a patient in a digital file that can be accessed by other physician colleagues? And what about when a physician overlooks a specific detail documented in the file? Can he be held legally responsible for doing so?
General practitioners thus remain rather hesitant to use sundhed.dk. Since 2013, however, patients have also had access – theoretically – to data contained in a so-called P-Journal. These are electronic health records that have been generated by general practitioners and other medical service providers such as physiotherapists, rehabilitation facilities or municipal nursing services. The number of physicians who create P-journals is growing, albeit slowly. One of the objectives delineated in Denmark’s current national E-Health Strategy is to increase access to P-journals.
“A Coherent and Trustworthy Health Network for All” is the title of the Danish government’s 45- page public dossier of its digital strategy for the next four years (2018-2022). Improving access to more data and enhancing the portal’s patient usability are just a few of the points targeted by the Danish government. Despite the considerable work ahead, when it comes to e-health, Denmark remains far ahead of the game in comparison to other countries.
Note: This blog post was written in cooperation with Cinthia Briseño. She supports on-site research for the survey #SmartHealthSystems with her journalistic contributions to our blog.
The study is carried out by empirica Communication and Technology Research on behalf of the Bertelsmann Stiftung.
Follow us as we take a closer look at e-health developments in various countries for our study throughout the course of 2018.
We will publish the full results of our international study in November 2018. Until then, we will be highlighting thought-provoking insights and best practices from other countries here in our blog. If you are interested in keeping up-to-date with our latest analyses, we recommend that you sign up for our email newsletter: